October 13 is World Thrombosis Day.
Thrombosis is a condition in which blood clots block the flow of blood. Clotting is triggered when a blood vessel is injured, when a blood vessel is compressed, or when clotting proteins in the blood are activated by other diseases, like an infection or inflammation. Cancer and its treatments commonly promote all three of these and can result in a life-threatening type of thrombosis called venous thromboembolism (VTE).

With approximately one in 200 patients diagnosed with cancer experiencing thrombosis and many dying due to VTE, Advancing Health Scientist Dr. Aggie Lee has dedicated much of her research program to understanding, preventing, and treating this serious complication.
VTE during cancer treatment
VTE occurs when blood clots block the flow of blood in a vein (deep vein thrombosis, DVT) or one of the lung’s arteries (pulmonary embolism, PE). Complete blockage of blood flow can then damage the tissues or a critical organ.
Throughout a patient’s cancer journey, their risk of having VTE varies. It is highest in the first few months after a cancer diagnosis and during chemotherapy treatment, targeted therapy, immunotherapy, and even hormonal therapy. There is also increased risk if major surgery is needed to remove the tumour, or if the cancer is growing and spreading to different parts of the body.
Dr. Lee, a Professor in the UBC Division of Hematology and Medical Director of the Vancouver Coastal Health (VCH) Thrombosis Program, emphasizes that a key step in preventing and treating thrombosis is accessing and using the most suitable anticoagulants for different patients.
“Anticoagulants, commonly referred to as blood thinners, are the cornerstone of treating blood clots. They prevent blood from clotting quickly and allow the body to break down clots that have been formed,” she said. “Having more options available for treating blood clots in patients with cancer means that we can personalize treatment to give them the best benefit-to-risk balance.”
In her recently published review paper, Dr. Lee and her colleagues compared the different anticoagulants available to treat patients. They proposed a step-wise approach to select the right medication for the job: 1) What is the risk of bleeding? The risk changes depending on the type of tumour, liver and kidney function, platelet count, and history of bleeding; 2) Are there possible drug-drug interactions that would make one anticoagulant better than another?; and 3) Are there any concerns with the stomach and intestinal tract that would interfere with the absorption of an oral anticoagulant?
Personalized treatment

With so many factors to consider, selecting the treatment that is safest and most effective for each patient can be complicated.
Jill Scott, a nurse on the VGH Thrombosis Clinic team within the VCH Thrombosis Program, works with patients to make sure they are educated about their thrombosis treatment.
“There are pros and cons to both oral and injected anticoagulants when treating and preventing VTE, but it is important to make sure the patient understands why their tailored anticoagulant prescription fits their cancer treatment,” said Jill. “When patients understand, we think they will do better.” Dr. Lee added.
For example, it may be more convenient to take a pill, but in some patients that might be associated with higher risks of serious bleeding, such as those with gastrointestinal cancers. Also, warfarin, a commonly prescribed oral anticoagulant, requires the patient to have regular, often weekly, blood tests to make sure that they are receiving the correct dose. For some patients, self-administering injection anticoagulants is safer, even though patients might be less comfortable injecting themselves. For example, this route is more suitable for patients with higher risks of serious bleeding, such as those with brain cancer or very low platelet counts, because the dose of an injectable anticoagulant can be adjusted easily. Sometimes, injection is the only option because of drug-drug interactions between oral anticoagulants and cancer medications.
Patient education
Thrombosis clinic nurses, including Jill, are responsible for educating patients, not only regarding their treatment options but also about cancer-related thrombosis in general. She also has personal experience with the importance of this type of patient education.
“The majority of cancer patients are not even aware that thrombosis is a potential complication from their cancer or during their treatment for cancer,” explained Jill. “When my sister was diagnosed with cancer, she was provided with a lot of information about her cancer treatment. There was only the briefest mention of the risk of thrombosis during one of the videos she had to watch. It did not emphasize that it is an important complication to be aware of.”

Even though the VGH Thrombosis Clinic has been treating cancer-related thrombosis for over a decade, the nurses and doctors have noted that it is very rare that patients know anything about thrombosis when they come to the clinic for treatment of DVT or PE. In fact, Dr. Lee has published research highlighting the need for better communication and a dedicated clinical pathway to help tackle mental distress from cancer-associated thrombosis. Educating patients about the possibility of experiencing VTE during cancer treatment is especially important as patients might mistake the signs and symptoms of thrombosis with the side effects of their cancer therapies.
“Thrombosis is a readily treatable condition when it is diagnosed early”, says Dr. Lee. “When the diagnosis is delayed or missed, treatment might be less effective and perhaps even dangerous. Patients with DVT might be left with a permanently swollen or painful leg from their DVT, or chronic shortness of breath from their PE. VTE has been shown to dramatically reduce quality of life as well as shorten survival in patients with cancer.”
Risks and signs of thrombosis
One of the reasons why cancer patients are at such high risk of VTE, aside from the cancer itself, is because many cancer treatments can trigger clotting and are delivered intravenously through indwelling central venous catheters which also promote clotting. It is important to note that some cancer treatments can cause blood clots regardless of whether or not it’s being administered via IV.
Additional risks include poor hydration, being very sedentary, and smoking. Some of the best ways to decrease the risk of VTE is to stay hydrated and remain as active as possible.
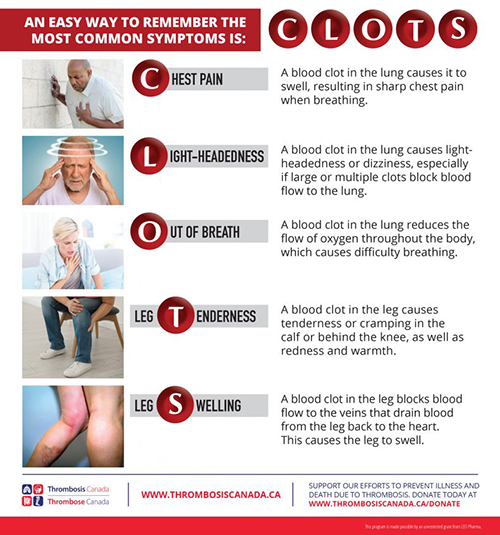
Although a cancer diagnosis can be overwhelming and patients receive a lot of information at once, it is important to educate them about the signs and symptoms of thrombosis.
“Knowing what the signs and symptoms of thrombosis are will help save lives,” Dr. Lee highlights. “Patients may otherwise ignore important signs and symptoms and not seek medical attention. Anticoagulants are highly effective medications, but doctors can only deliver them when a diagnosis is made. How early that happens is entirely dependent on the patient’s awareness and seeking help.”
More information
Feel free to watch a video from Thrombosis Canada sharing signs and symptoms of cancer-associated thrombosis.
Also, please visit Thrombosis Canada and the VGH Thrombosis Clinic websites for more information.



