The Evidence Speaks Series is a recurring feature highlighting the latest in CHÉOS research. This series features summaries of select publications and is designed to keep media and the research community up to date with CHÉOS’ current research results in the health outcomes field.
To ensure this research is quick and easy to share, we are now providing social cards that you are free to save and use as you see fit.
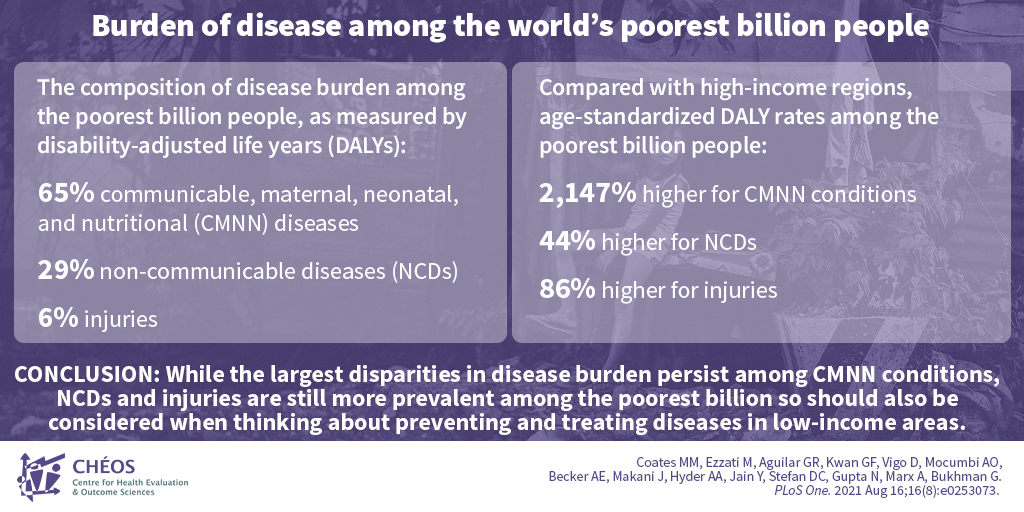
Understanding disease burden among the poorest people in the world
Coates MM, Ezzati M, Aguilar GR, Kwan GF, Vigo D, Mocumbi AO, Becker AE, Makani J, Hyder AA, Jain Y, Stefan DC, Gupta N, Marx A, Bukhman G. Burden of disease among the world’s poorest billion people: An expert-informed secondary analysis of Global Burden of Disease estimates. PLoS One. 2021 Aug 16;16(8):e0253073.
CHÉOS Scientist Dr. Daniel Vigo joined researchers from across the globe to determine disease burden among the world’s poorest billion people compared to high-income populations. Among the poorest billion, 65 per cent of diseases were communicable, maternal, neonatal, and nutritional (CMNN), 29 per cent were non-communicable (NC), and 6 per cent were injuries. The burden of all three categories was significantly higher among the poorest billion compared with high-income populations, as measured by age-standardized disability-adjusted life years: 2,147 per cent higher for CMNN diseases, 44 per cent higher for NC diseases, and 86 per cent higher for injuries. These results show that the largest disparities in disease burden are in CMNN conditions; however, injuries and NC diseases remain important factors to consider when thinking about preventing and treating diseases in low-income areas.
—
Resuscitation via intraosseous access in pediatric OHCA is associated with lower chance of survival
Besserer F, Kawano T, Dirk J, Meckler G, Tijssen JA, DeCaen A, Scheuermeyer F, Beno S, Christenson J, Grunau B, on behalf of the Canadian Resuscitation Outcomes Consortium. The association of intraosseous vascular access and survival among pediatric patients with out-of-hospital cardiac arrest. Resuscitation. 2021 Aug 10 epub ahead of print.
CHÉOS Scientists Drs. Brian Grunau and Jim Christenson, Emergency Medicine Program Head Dr. Frank Scheuermeyer, and investigators from the Canadian Resuscitation Outcomes Consortium studied the effect of intraosseous (IO) and intravenous (IV) access on outcomes in pediatric out-of-hospital cardiac arrest (OHCA). Reviewing data from 1,549 OHCAs in patients aged 17 and under, the team discovered that 895 patients had an IO line attempted with 822 being successful, while 488 had an IV line attempted with 345 being successful. The researchers then conducted a logistic regression analysis with 761 patients to determine the association between access method and survival. Of these patients, 601 received IO access and 160 received IV access. Only 5.2 per cent of patients who received IO access survived compared with 25 per cent of patients who received IV access. The research team concluded that IO access was associated with a lower chance of survival and more research is needed into the impact of IV access on pediatric OHCA outcomes.

—
Psychosocial support could benefit living kidney donors in the month’s after surgery
Garcia-Ochoa C, Feldman LS, Nguan C, Monroy-Caudros M, Arnold JB, Barnieh L, Boudville N, Cuerden MS, Dipchand C, Gill JS, Karpinski M, Klarenbach S, Knoll G, Lok CE, Miller M, Prasad GVR, Sontrop JM, Storsley L, Gargand AX, For the Donor Nephrectomy Outcomes Research (DONOR) Network. Impact of Perioperative Complications on Living Kidney Donor Health-Related Quality of Life and Mental Health: Results From a Prospective Cohort Study. Can J Kidney Health Dis. 2021 Aug 11 epub ahead of print.
CHÉOS Scientist Dr. John Gill and colleagues conducted a prospective cohort study to understand the impact of perioperative complications on Canadian living kidney donors’ health-related quality of life (QoL), depression, and anxiety. Of the 912 living kidney donors enrolled in the study, 74 experienced a perioperative complication; the vast majority of these were minor and resolved before they left hospital. Using the Beck Anxiety Inventory and Beck Depression Inventory, which each contain 21 questions on symptoms of anxiety and depression, respectively, the researchers determined that a perioperative complication was not associated with changes in anxiety, but was associated with higher depression symptoms three months after donation. They also found that although mental health-related quality of life worsened three months after surgery, physical health-related quality of life was not impacted. The results of this study highlight the potential need for psychosocial support in the months following surgery for donors who experience complications.




