
People tend to have diverse reactions when seeing blood. Some faint, some feel squeamish, some are curious, and a very select few fall in love. That is exactly how new CHÉOS Scientist Dr. Aggie YY Lee felt when she was first introduced to hematology — the study of the physiology of blood.
“During my third year in medical school, I did an elective in hematology and by the end of my first afternoon, I was absolutely fascinated. It was love at first sight!” shares Dr. Lee, who just happened to be born the same year that the blood clotting cascade was discovered. Destiny? “Hematology is a very diagnostic field. In hemostasis and thrombosis, I have to figure out why a patient’s blood may not be clotting or is clotting excessively. It’s a puzzle, and as someone who likes to solve problems, I found that hematology really suited me.”
True beauty
Another facet of hematology that Dr. Lee finds very appealing is the visual aspect of the work. In both medicine and research, so much important information is represented by numbers, such as measurements, ranges, or tables. To help understand what is going wrong in a patient’s blood, hematologists get to actually look at the blood smears and samples from patients.
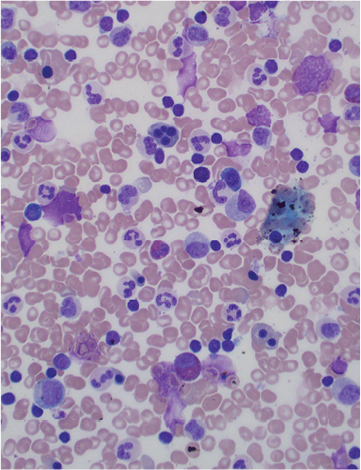
“I just love looking at blood cells and the bone marrow; it is so pretty. I used to wish that I had wallpaper of normal blood marrow because it’s so beautiful.” Dr. Lee expands, “It is also wonderful to see what’s actually going on in the body and that’s part of why I enjoy this work. A picture says a thousand words, it gives that additional dimension. Hematology offered a whole new world to me, with so many fascinating facets, including the coagulation cascade that just spoke to me and made sense. Everything fit for me.”
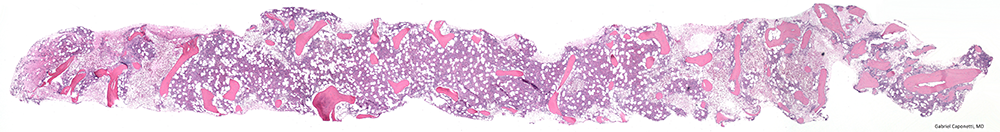
There will be research
Dr. Lee didn’t always know that she was going to enjoy working with blood. When starting medical school, she intended to become a neurosurgeon but found that the environment didn’t suit her personality. She wasn’t even initially interested in research, but was offered a thrombosis research fellowship at McMaster University, internationally recognized for its excellence in thrombosis. This fellowship was her initial foray into research methodology training, where Dr. Lee learned to design clinical trials and obtained her Master’s degree.
“I fell into research, it wasn’t a planned career, but after the training to design research studies, I really fell in love with clinical research and the work I was doing,” says Dr. Lee, who is also the Medical Director of the Thrombosis Program and Professor of Medicine at UBC.
Currently, she is working with colleagues on a clinical trial looking at a new class of small molecular anti-coagulants that could be very effective in treating blood clots without the burden of causing bleeding. Dr. Lee explains, “I work largely with patients with cancer, who have high risks of clotting and bleeding. So, when they have to be treated with anticoagulants to block clotting, we have a double-edged sword, because bleeding is almost a necessary side effect. Previously, we have never been able to dissociate clotting and bleeding using anticoagulants, but now we are looking at novel agents that may actually be able to separate these two phenomena. The preliminary data show that these drugs could reduce a patient’s risk of thrombosis without increasing the risk of bleeding by blocking clotting factors higher up in the clotting cascade.”
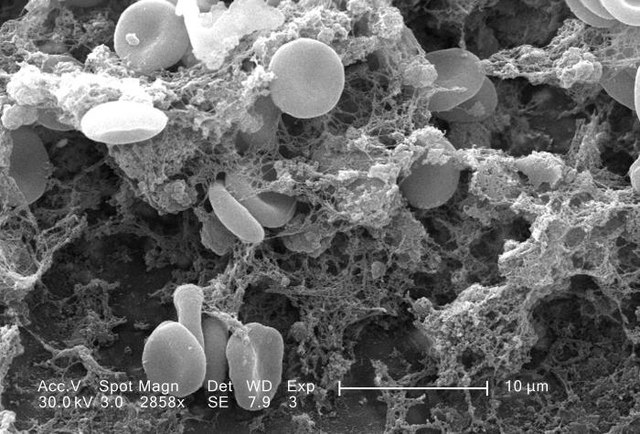
Dr. Aggie Lee and the full-blood patient
In addition to research, Dr. Lee also enjoys talking with her patients. “One thing I didn’t expect was how much your patients actually teach you. If you listen to your patients, they teach you an incredible amount about their treatment. They have helped me, not only by sharing their signs and symptoms but also their experiences. It has made a huge difference over the years because it helps me identify gaps in their care and has made me better at what I do.”
Communicating with patients is important and something kept top of mind is that doctors can often speak a different language. She recalls a story from her fourth year in medical school, “I was late to meet my husband one evening, and I explained that I had to stay and attend to a patient who had ‘spiked a temp’. It turns out my husband thought that ‘spiked a temp’ meant a patient stabbed a temporary worker. In medicine, spiking a temp is a way to say that a patient had a fever. After that miscommunication, I always think about how I speak to people who are not in medicine, especially when trying to explain things to patients about their diagnosis and treatment.”
Another experience Dr. Lee had that emphasized the importance of patient communication happened in residency when she tried translating for a patient speaking Cantonese. As someone who spoke Cantonese fluently at 10 years old, before moving to Canada and learning English, she was asked to help the patient understand that he had been diagnosed with hepatitis — inflammation of the liver.
“When I was asked to translate, I thought ‘well, I can speak Cantonese and I know the Cantonese words for inflammation and for liver.’ However, what I effectively told him was that he had ‘inflammation of his pâté’ because I used the word for liver in Cantonese that describes it as a food item, similar to how we say beef for cow and pork for pig. The patient was a bit taken back and then we had a good laugh when he explained what I said. After that, I tried to leave the translating to the professionals.”
If you want talks (you got them)
As an active researcher, Dr. Lee not only communicates with her patients but also presents her research at conferences all over the world. With hundreds of presentations worth of experience, one wouldn’t think a fear of public speaking would be an issue.
“I had a bad childhood experience at a Christmas pageant when I was six. It was my first experience on stage and my costume didn’t fit properly and I ended up having a wardrobe malfunction,” recalls Dr. Lee. “Since then, I get palpitations when I get on the stage to speak. Plus, English is my second language, and that also adds to my fear of public speaking. When I am tired or nervous, I am aware of my accent and my English grammar falls apart.”
Even with this fear, she has powered through and, prior to the pandemic, was giving presentations at one or two conferences per month. Public speaking is a huge part of sharing her work and, even though she still gets palpitations before speaking, her passion for her work empowers her.
The recipe for success
What else is Dr. Aggie Lee passionate about?
Finding the perfect shortbread recipe!
Although she doesn’t identify as a baker, Dr. Lee loves making shortbread, “I’ve been trying different shortbread recipes. I’m a bit of a perfectionist but also very busy so I’m looking for a recipe that’s minimal in effort but maximal in how good the cookies look. Plus, of course, they have to be delicious!”
She emphasizes the importance of finding something that you love doing. “Time flies when you’re having fun. I’ll be working hours and hours on something thinking that only five minutes have passed. Because I enjoy what I’m doing, I never think of it as a chore or a burden.”
Even though Dr. Lee didn’t intend on becoming a hematologist, she was always open to opportunities.
“I know it’s a cliché, but when life gives you lemons, make lemonade. I didn’t plan on doing research or thrombosis but because I was granted a thrombosis fellowship, I made the best of the situation and it gave me a career that I love. Even though I still get nervous with public speaking, I’m excited to share my research. There are a lot of things that ended up being unplanned success stories because I didn’t have blinders on. It’s important to both notice and be open to other opportunities. Being a good doctor and a good researcher requires making observations, following up with inquisitive questions, and then searching for answers.”


